An investigation by the BBC has revealed that unsafe medical practices continued at a government hospital in Punjab months after it was linked to a major HIV outbreak among children, raising serious concerns about infection control and systemic failures in healthcare.
The findings, published by BBC Eye, centre on Tehsil Headquarters (THQ) Hospital in Taunsa, where a surge in paediatric HIV cases was first identified in late 2024 by doctors at private clinics who noticed an unusual pattern among affected children.
Among the victims was eight-year-old Mohammed Amin, who died shortly after testing positive. His mother recalled his severe fevers and pain, while his sister Asma, who also contracted HIV, continues to battle the disease. Facing stigma, she has asked her family: “What is wrong with me?”, as neighbours prevent their children from playing with her.
Authorities acknowledged the outbreak in early 2025, confirming 106 infections and promising a “massive crackdown”, suspending the hospital’s medical superintendent in March that year.
Officials in Dera Ghazi Khan said that most of the HIV cases among children in Taunsa date back to last year, according to Deputy Commissioner Muhammad Usman Khalid. He added that health department teams are continuing investigations into the outbreak, while affected children have been registered and are receiving treatment.
The deputy commissioner also said that authorities carried out crackdowns against unqualified medical practitioners in Taunsa and Dera Ghazi Khan, sealing 275 illegal clinics over the past year. “There is currently no unqualified practitioner operating,” he said, adding that no one would be allowed to play with people’s lives.
However, undercover filming carried out over several weeks in late 2025 found that dangerous practices were still ongoing.
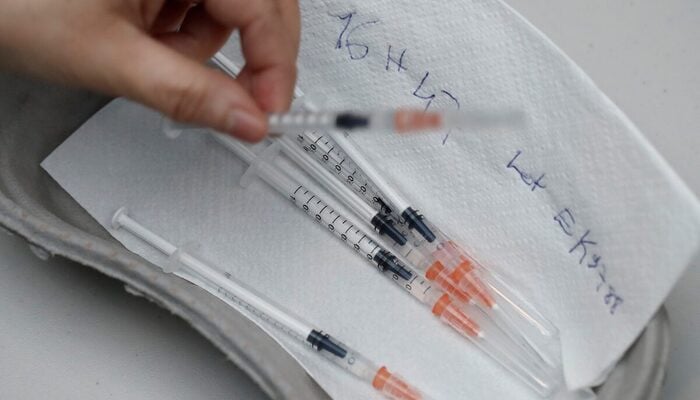
Investigators documented syringes being reused on multi-dose vials at least 10 times, with medicine from the same vial administered to different children in four instances. Staff were also filmed injecting patients without sterile gloves on 66 occasions.
In one instance, a nurse was seen retrieving a used syringe containing liquid from a previous patient and handing it to a colleague, apparently for reuse. In others, unqualified volunteers — officially banned from the ward — were seen administering injections to children.
Experts warned that such practices pose a severe risk of infection. Dr Altaf Ahmed said contaminated syringes could transmit viruses even if needles were changed, as the syringe body itself could carry infection.
The investigation also highlighted that many children were being treated via cannulas — tubes inserted directly into veins — increasing the likelihood of infection as contaminated substances can enter the bloodstream without natural barriers.
Data compiled by the broadcaster showed that at least 331 children in Taunsa tested positive for HIV between November 2024 and October 2025. Among families tested, fewer than one in 20 parents were HIV-positive, suggesting most infections were not due to mother-to-child transmission. At least 19 new cases have been detected in recent months, and at least nine children have died.
A leaked inspection report by health authorities, alongside the World Health Organisation and Unicef, found conditions “especially concerning” in the paediatric emergency ward, citing reused IV fluids, unlabelled cannulas, used IV sets left hanging, and a lack of basic hygiene facilities, including sanitisers.
Despite this, officials denied conclusive responsibility. The current medical superintendent, Dr Qasim Buzdar, rejected the undercover footage, suggesting it may have been staged or filmed before his tenure, while maintaining that infection control measures were in place. His predecessor, Dr Tayyab Chandio, also denied that the hospital was the source of the outbreak.
The BBC findings also pointed to a wider pattern. In Karachi’s SITE Town, dozens of children — including two-year-old Mikasha — tested positive for HIV after treatment at a government hospital, with authorities later confirming that reused contaminated syringes had triggered at least 84 cases.
Health experts say the crisis reflects deeper systemic issues, including widespread reliance on injections as treatment. Pakistan has one of the highest rates of therapeutic injections globally, many of them unnecessary, driven by patient demand and accepted practice among doctors.
Shortages of medicines and supplies further exacerbate the problem, forcing staff in overstretched public hospitals to reuse equipment or share medication between patients.
For families like Asma’s, however, the consequences are lifelong. While medication keeps her alive, the stigma surrounding HIV has left her isolated. Despite this, she says she studies hard and hopes to become a doctor one day — a future shaped by a disease she may never have been exposed to under safe medical care.